UCLA Mobile Stroke Unit saves time, provides lifesaving care on the scene
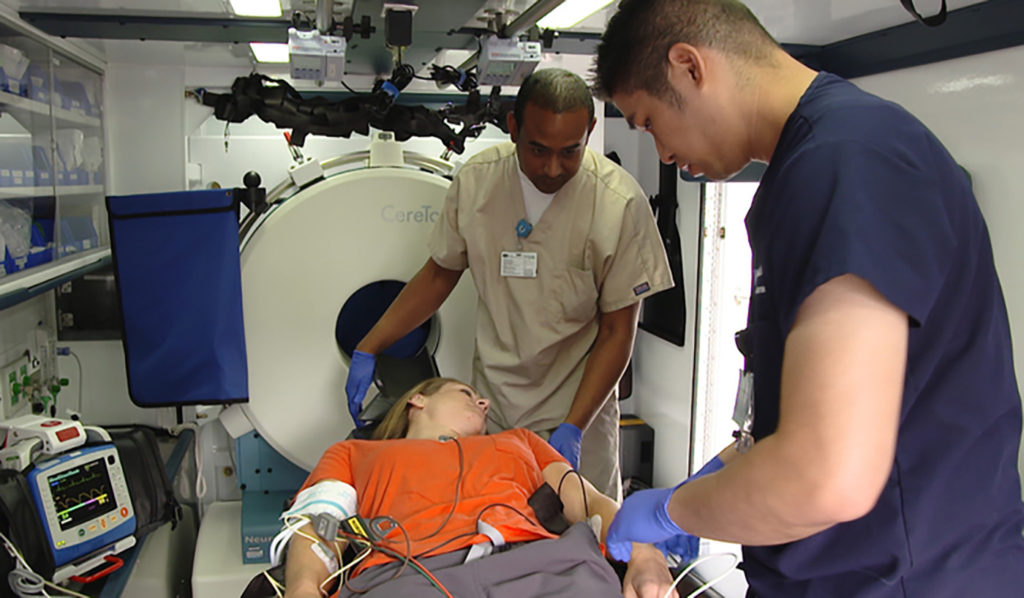
The UCLA Mobile Stroke Unit is working to improve care for stroke victims by reducing the time between diagnosis and treatment. (Noah Danesh/Daily Bruin)
By Noah Danesh
Feb. 10, 2021 12:58 p.m.
This post was updated Feb. 15 at 09:27 p.m.
A UCLA program is aiming to improve stroke care by providing treatment for stroke victims out of a mobile unit that can diagnose and treat them in the field.
The UCLA Mobile Stroke Unit is a specialized ambulance with a medical team on board that is equipped with tools to diagnose and treat strokes, including a mobile CT scanner, said Dr. May Nour, the medical director for the Arline and Henry Gluck Stroke Rescue Program, which runs the stroke unit.
UCLA’s MSU, founded in 2017, is dispatched from three areas in Los Angeles County to 23 cities in the county. There is currently one unit – staffed with a vascular neurologist, CT technologist, critical care nurse and paramedic – that responds to the cities on a rotating basis, but Nour said she hopes to expand to multiple units to cover the county.
Speed is essential when treating strokes, said Nour, who is also a UCLA neurologist. Two million brain cells die every minute during an ischemic stroke, which is when a blood vessel is blocked, she added.
The MSU can save an average of 30 to 45 minutes by providing treatment in the field, Nour said.
When somebody calls 911 with reports of the signs of a stroke, both the MSU and normal emergency medical services are dispatched. Once they arrive on scene, the medical teams use the diagnostic tools to determine whether the patient is experiencing a stroke.
“Time loss is brain loss,” Nour said. “What we would like to do is to immediately diagnose the patient in a conclusive way and give them the life and brain-saving treatments immediately, prior to transporting them to the hospital.”
Nour said that when members of the MSU diagnose someone with an ischemic stroke, they can provide the proper treatment – a clot-busting medication called tissue plasminogen activator or tPA.
“Mobile stroke units, in essence, bring the hospital to the patient,” she said.
Soumya Ravichandran, a third-year psychobiology student who is a member of the UCLA Student Stroke Force, a student organization that assists in stroke research at the emergency department, said that by providing care at the scene, the MSU is able to effectively shorten the time it normally takes in an emergency room. Typically, patients need to receive a stroke diagnosis once they arrive at the emergency room before receiving treatment.
Nour added that the COVID-19 pandemic affected the nature of stroke calls – more patients delay their calls to 911 because of COVID-19.
“They are afraid to call 911. They are afraid to come to the hospital,” Nour said.
The MSU may free up EMS units to respond to other calls, which has become important during the pandemic as EMS resources are being strained, Nour said.
UCLA’s MSU was launched with a donation from the Arline and Henry Gluck Foundation and was the first unit of its kind in California. UCLA also received a $1 million donation in December to support a nursing fellowship for the MSU.
When the unit is unavailable, paramedics follow the normal protocols of transporting patients to stroke-approved hospitals, said Walter Gonzalez, a firefighter paramedic from the Santa Monica Fire Department who works with the MSU.
The MSU is part of a national research study of stroke units, called BEST-MSU. The results of the study will likely be presented at the International Stroke Conference in March and could show whether the unit improves patient outcomes and is cost-effective, Nour said.
LA County approved $1.4 million of additional funding for the MSU in September, which will allow the program to run through the end of 2021 while it tries to attain insurance funding, according to a LA County press release.
Once the additional research about the MSU is presented in March, Nour said she hopes insurance companies will cover the stroke treatment in the unit the same way it is covered when provided at emergency departments.
While the research is still underway, Gonzalez said he thinks the MSU has impacted people who get the tPA treatment in a positive way.
Andy Reno, an EMS coordinator for the Long Beach Fire Department, said he believes the stroke unit is a valuable resource for the city.
“The positive outcome on patient care is amazing,” he said. “To be able to get those services to the patient immediately, wherever they are on scene, is amazing.”
